  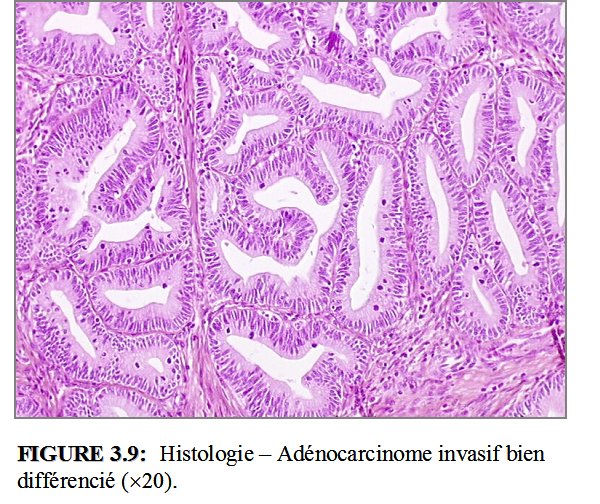
on behalf of the International Society of Gynecological Pathologists. In addition, this article addresses the distinction of human papilloma virus-associated adenocarcinoma in situ and gastric type adenocarcinoma in situ from their invasive counterparts.Ĭopyright © 2021 International Society of Gynecological Pathologists. Moreover, the current National Comprehensive Cancer Network (NCCN) guidelines include this classification as an "emergent concept." In order to facilitate the understating and application of this new classification by all pathologists, the ISGyP Endocervical Adenocarcinoma Project Working Group presents herein all the current evidence on the Silva classification and aims to provide recommendations for its implementation in practice, including interpretation, reporting, and application to biopsy and resection specimens. Although not a part of any staging system yet, it has been incorporated in synoptic reports as established by the College of American Pathologists (CAP) and the International Collaboration on Cancer Reporting (ICCR). Should clinical outcomes and genomic studies continue to support these findings, we recommend replacement of the World Health Organization 2014 criteria with the IECC 2017.The Silva pattern-based classification for human papilloma virus-associated invasive adenocarcinoma has emerged as a reliable system to predict risk of lymph node metastasis and recurrences. Endometrioid and serous carcinomas of the endocervix are extraordinarily rare. This study confirms that usual-type ECAs are the most common type worldwide and that mucinous carcinomas comprise a mixture of HPVA and NHPVA, with gastric-type carcinoma being the major NHPVA type. IECC reliably segregates ECAs into HPVA and NHPVA types using morphology alone. The high-risk HPV chromogenic in situ hybridization probe set had superior sensitivity, specificity, and positive and negative predictive values (0.955, 0.968, 0.992, 0.833, respectively) compared with p16 immunohistochemistry (0.872, 0.632, 0.907, 0.545, respectively) to identify HPV-related usual carcinoma and mucinous carcinoma. NHPVA tumors were larger and occurred in significantly older patients, compared with HPVA tumors (P<0.001). The 1 HPV gastric-type carcinoma was found to have hybrid HPVA/NHPVA features on secondary review. When excluding cases thought to have suboptimal tissue processing, 90% and 95% of usual-type IECC cases overexpressed p16 and were HPV, whereas 37% and 3% of NHPVAs were p16 and HPV, respectively. Only 3 endometrioid carcinomas were recognized and all were NHPVA. The 5 most common IECC diagnoses were usual-type (HPVA) (73% of cohort), gastric-type (NHPVA) (10%), mucinous adenocarcinoma of HPVA type, including intestinal, mucinous not otherwise specified, signet-ring, and invasive stratified mucin-producing carcinoma categories (9%), clear cell carcinoma (NHPVA) (3%) and adenocarcinoma, not otherwise specified (2%). Tissue microarrays representing 297 cases were constructed immunohistochemistry (p16, p53, vimentin, progesterone receptor) and chromogenic in situ hybridization using an RNA-based probe set that recognizes 18 varieties of high-risk HPV were performed to validate IECC diagnoses. Most tumours develop from a non-invasive type of cancer called endocervical adenocarcinoma in situ (AIS). It develops from glandular cells normally found in a part of the cervix called the endocervical canal. Complete slide sets from 409 cases were collected from 7 institutions worldwide. Endocervical adenocarcinoma is a type of cervical cancer. HPVAs were then subcategorized based on cytoplasmic features (mostly to provide continuity with preexisting classification schemes), whereas NHPVAs were subclassified based on established criteria (ie, gastric-type, clear cell, etc.). The International Endocervical Adenocarcinoma Criteria and Classification (IECC criteria), described herein, distinguishes between human papillomavirus-associated adenocarcinoma (HPVA), recognized by the presence of luminal mitoses and apoptosis seen at scanning magnification, and no or limited HPVA features (nonhuman papillomavirus-associated adenocarcinoma ). We sought to classify endocervical adenocarcinomas (ECAs) based on morphologic features linked to etiology (ie, human papillomavirus infection), unlike the World Health Organization 2014 classification. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
